De-Risking the Path to Cell & Gene Therapy Commercialization Part 1: You Need Access to a Robust and Reliable Donor Pool
When cell and gene therapy researchers step into the lab each morning, we envision transforming what may be an early stage experiment into a clinical success. Therapeutics developers spend years working tirelessly to generate pre-clinical data so that, when the time comes, their Investigational New Drug (IND) application (or equivalent outside the USA) will be accepted by the appropriate regulatory agency, allowing the therapy to enter clinical trials. However, IND approval is just the first of many significant hurdles that therapeutics developers face on the path to commercialization.
Although treating patients may seem far off, it’s never too early to begin preparing. Selecting raw materials suppliers who can provide a continuous and reliable supply of both research and cGMP grade resources, supporting a program from pre-clinical development through clinical trial manufacturing (if not into commercialization), is one of the most important things a researcher with aspirations for the clinic can do early on to set the stage for success.
This series of Supply Brain posts will address means of mitigating supply chain challenges associated with the clinical translation of a cell-based therapy; this one focuses on issues surrounding donor variability. You can find facts about current Good Manufacturing Practices (cGMPs) from the US FDA here. More on cGMP compatibility, reproducibility, and scalability to come in subsequent posts.
Research and pre-clinical development are often conducted with research grade cells. These materials are not regulated by the FDA and are therefore labeled “For Research Use Only (RUO)”. However, the FDA, and most regulatory agencies worldwide, have stringent requirements for human cells, tissues, and cellular and tissue-based products (HCT/Ps) that will be used in treating humans, and many guidance documents exist to inform developers of these regulations.
For one, the quality, safety, and consistency of biological raw materials (including cytokines, growth factors, sera, antibodies, plasmids, etc.) used in cell manufacturing must be documented and provided for regulatory review. Not only are quality attributes such as identity, purity and potency/biological activity (including variability) of these materials and the final cell or gene product important, but there also must be information provided on origin, traceability and viral safety.
As a result, the supply chain for cellular starting materials is confounded by even more challenges than those for other biologics, due to the source: human donors. Material sourced from humans is inherently variable due to individual donor differences. To further complicate the issue, organs, tissues, and cells are also complex, heterogeneous systems with inherent variability.
It is essential to partner with suppliers that manage their own donor pool and who will work with you to continuously improve upon critical material attributes for your starting materials.
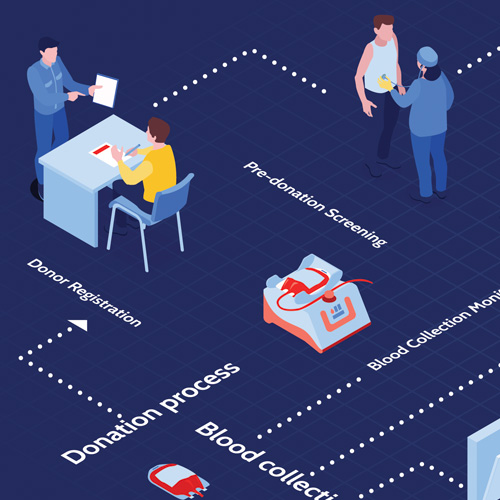
While setting up your own supply chain is doable, donor recruitment, qualification, and maintenance are no small tasks. Dedicated resources and individuals are needed to manage your donor pool. This requires a host of activities from gaining Institutional Review Board approval to ensure safety of human subjects, to consenting patients and taking their medical history to determine safety and eligibility, to managing logistics around sample/tissue collection, transport, storage, and processing. More on this in a follow-on blog post.
Maintaining a large and diverse donor pool is, however, critical to success. A donor’s age, race/ethnicity, weight, health, disease status, and lifestyle (for instance, does he/she smoke?) all affect the quality and functionality of the tissues and cells he/she donates.
The collection process can also affect quality and consistency of the tissue/cell product, so having direct relationships that allow you to train physicians who are obtaining tissues on your behalf is also important. In fact, when it comes to birth tissues, whether the birth process itself is high stress or low stress may influence the total nucleated cell count and the prevalence of progenitor cells in umbilical cord blood, so the donor experience is also important to consider and manage, to the extent possible.
Much as we set product specifications, being able to extend that to donor specifications can aid the success of process and product development efforts, or at the very least, yield significant data points on what may and may not affect your process and final product. Many in the industry are embracing Quality by Design (QbD) approaches that account for such considerations in product development.
So, what should you do if you cannot generate and manage your own donor pool? Outsource to a suitable supplier. In such a case, it is essential to partner with reliable suppliers who have established, dedicated supply chains from donor pools that they manage.
Not only does this allow you to have better control over your cell therapy product starting materials, but it also gives you the ability to request cells from multiple donors so that you can study the effects of donor variability on your process and product. Whether your therapy is autologous or allogeneic, it is essential that you understand the effects donor-based differences have on your process and final product.
Accounting for donor variability early in the process and product development lifecycle is critical to the success of your program. Doing so increases the consistency and reproducibility of your product and allows you to clearly identify the necessary donor attributes for future starting materials.
To this end, seek suppliers with whom you may continuously improve upon critical material attributes for your starting cellular raw materials.
Having access to a robust and reliable donor pool is the foundation upon which successful cell and gene therapies are built, and this is why every aspect of OrganaBio’s supply chain is proprietary and controlled by us.
This includes everything from donor recruitment, for the procurement of birth tissue, to the isolation of mesenchymal stromal (MSCs) and immune cells for research and clinical applications. By leveraging our supply chain, our customers have confidence that their cell supply is stable, robust, high quality and clinically relevant.